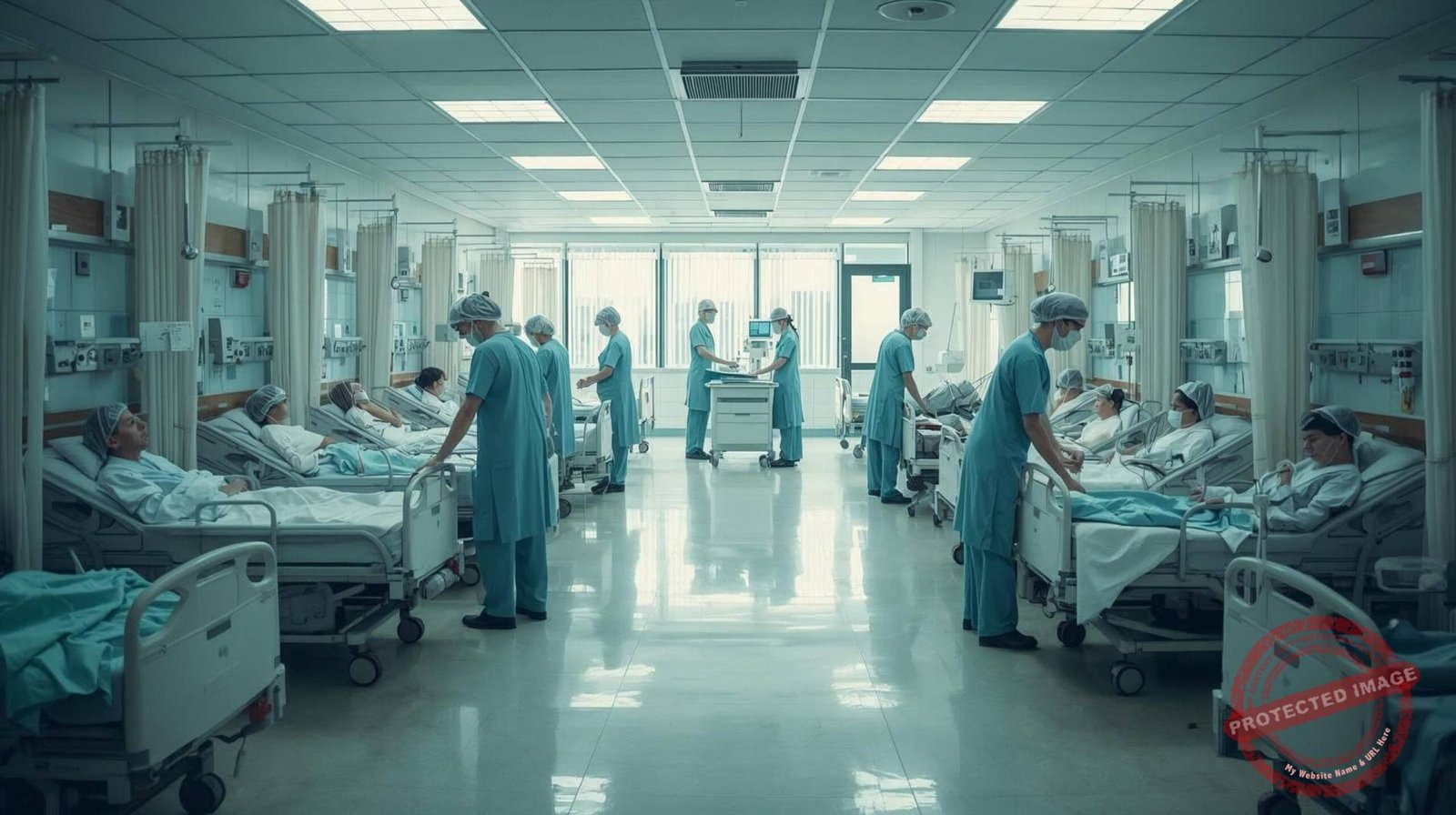
Cohortoring in nursing is an infection prevention strategy that involves grouping patients colonized or infected with the same infectious agent (e.g., COVID-19, MRSA, VRE) together to confine their care to a specific, dedicated area and staff, thereby preventing the spread of pathogens to uninfected patients. It is typically utilized when single-patient rooms are unavailable or during outbreaks.
Here are the key guidelines for cohorting in nursing:
1. Patient Selection and Placement
- Confirmed Infection: Cohort only patients with a confirmed, identical laboratory diagnosis.
- Avoid Mixed Cohorts: Do not mix patients with different infections (e.g., COVID-19 with Influenza).
- Exclude “Under Investigation”: Patients under investigation (PUIs) for a disease should not be cohorted with confirmed cases.
- Spatial Separation: Beds in multi-occupancy rooms should be separated by at least 6 feet.
- Barriers: Physical barriers (e.g., curtains, screens) must be in place and closed at all times.
- Room Requirements: Doors to the cohort room should remain closed.
2. Staffing Assignments
- Dedicated Personnel: Assign specific nurses and healthcare personnel (HCP) to care only for the cohorted patients.
- Avoid Floating: Staff should not rotate between cohorted (infected) areas and non-cohorted (clean) areas.
- “Well to Ill” Flow: If staff must work in both areas, they should care for uninfected patients before moving to the infected cohort.
3. Infection Control Measures
- PPE Adherence: Strict adherence to Personal Protective Equipment (PPE) is mandatory. Change gloves and gowns between patient interactions within the cohort room.
- Hand Hygiene: Perform hand hygiene before and after all patient contact, particularly when moving between patients in a shared room.
- Equipment Dedication: Dedicate equipment (e.g., thermometers, blood pressure cuffs) to the cohort area or individual patient, or thoroughly disinfect between uses.
- Environmental Cleaning: Increase the frequency of cleaning and disinfection for surfaces in the cohort area.
4. Administrative and Safety Considerations
- Gender Separation: Generally, only patients of the same gender should be cohorted, unless they are family.
- Age Separation: Do not cohort children with adults unless they are from the same household.
- Visitation: Limit or eliminate visitors in cohorted rooms to minimize exposure risk.
- Communication: Clearly communicate the rationale for cohorting to patients and families.
5. Long-Term Care (LTC) Specifics
- Separate Units: Designate entire wings, units, or floors as “isolation units” for infected residents.
- Separate Entrances: Ideally, the cohort unit should have a separate entrance.
- Monitor Trends: Maintain a daily log of resident infections to quickly identify and cohort new cases.
If a single room is not available during a surge, cohorting is considered a necessary, temporary, and effective method to stop further transmission within a facility.