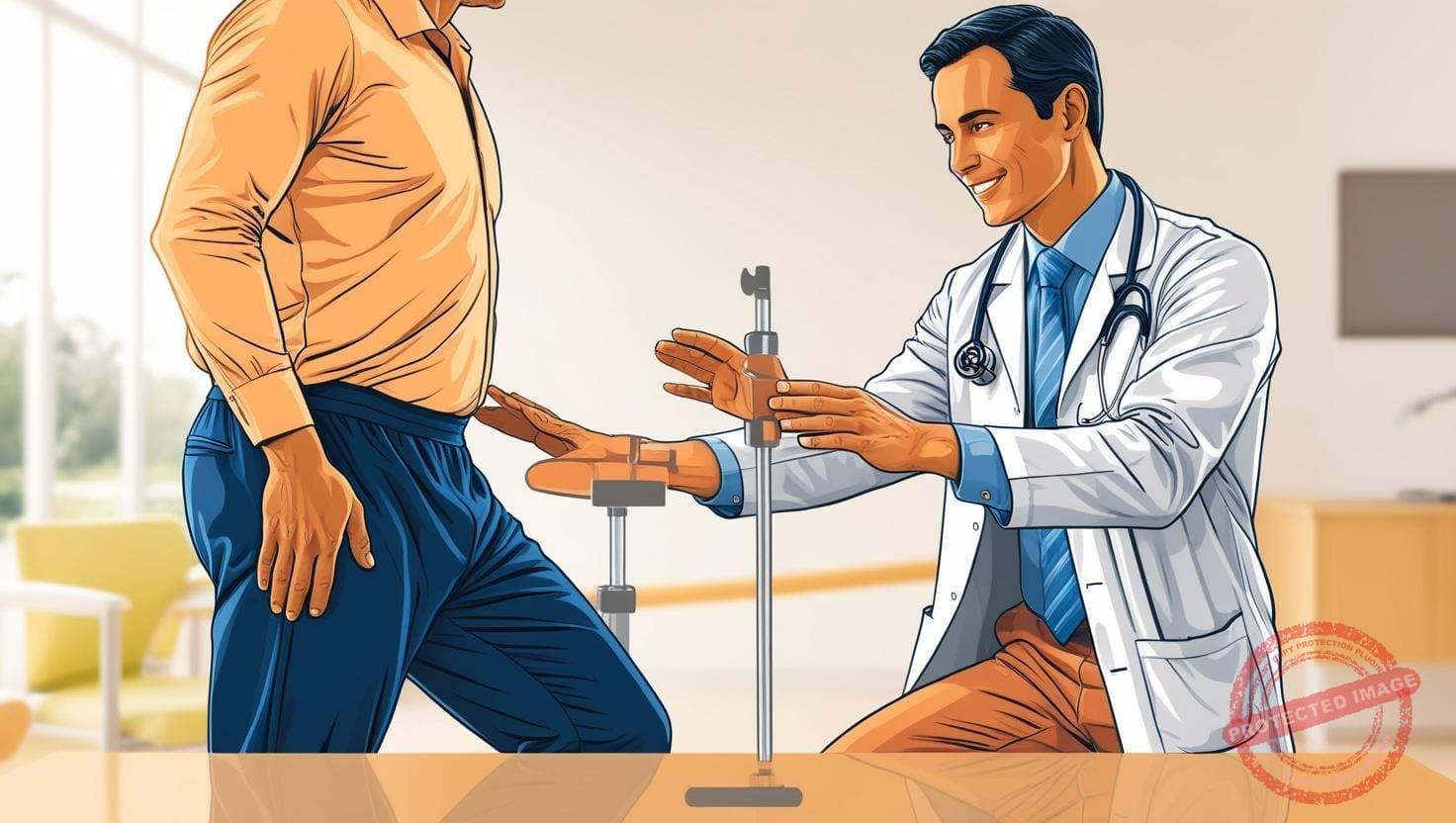
Gait evaluation is a critical part of the physical examination, providing valuable insights into musculoskeletal, neurological, and systemic conditions. A systematic approach includes assessing the patient’s walking pattern, analyzing components of gait, and identifying abnormalities.
Normal Gait
Gait involves a cycle of movements with two phases for each leg:
- Stance Phase (60% of gait cycle):
- Foot is in contact with the ground.
- Subdivided into heel strike, mid-stance, and toe-off.
- Swing Phase (40% of gait cycle):
- Foot is off the ground, moving forward.
- Subdivided into initial swing, mid-swing, and terminal swing.
- Key Features:
- Symmetry, rhythm, and efficiency.
- Proper coordination of arm swing and trunk movement.
Steps of Gait Evaluation
1. Observation
- Walking Pattern:
- Observe from front, back, and side views.
- Note step length, stride, rhythm, and symmetry.
- Arm Swing:
- Normal gait includes reciprocal arm movement.
- Posture:
- Look for leaning, tilting, or unusual positions.
- Foot Placement:
- Evaluate alignment and any inward/outward rotation.
2. Specific Gait Components
- Stance and Stability:
- Ability to maintain an upright position.
- Stability during single-leg stance.
- Balance and Coordination:
- Assess for unsteadiness or swaying.
- Speed and Cadence:
- Normal cadence: ~90–120 steps per minute.
- Slow or fast gait may indicate neurologic or musculoskeletal issues.
3. Provocative Maneuvers
- Heel-to-Toe Walking:
- Tests cerebellar function and coordination.
- Tandem Gait:
- Walking in a straight line heel-to-toe.
- Toe Walking:
- Evaluates strength and function of the gastrocnemius and soleus.
- Heel Walking:
- Tests dorsiflexor strength (e.g., anterior tibialis).
Common Gait Abnormalities
| Gait Type | Characteristics | Associated Conditions |
|---|---|---|
| Antalgic Gait | Shortened stance phase on the painful side. | Pain (e.g., arthritis, fractures). |
| Trendelenburg Gait | Hip drops on the contralateral side during stance phase. | Weak gluteus medius (e.g., hip dysplasia, neuropathy). |
| Steppage Gait | Exaggerated hip and knee flexion to clear the foot; foot slap upon contact. | Foot drop (e.g., peroneal nerve injury). |
| Spastic Gait | Stiff, scissoring legs, circumduction of affected limb. | Upper motor neuron lesions (e.g., stroke, CP). |
| Ataxic Gait | Wide-based, unsteady gait with irregular step rhythm. | Cerebellar dysfunction (e.g., stroke, alcohol use). |
| Parkinsonian Gait | Shuffling steps, stooped posture, reduced arm swing, difficulty initiating movement (“freezing”). | Parkinson’s disease. |
| Waddling Gait | Rolling hip movement, exaggerated lumbar lordosis. | Proximal muscle weakness (e.g., Duchenne muscular dystrophy). |
| Apraxic Gait | Difficulty initiating walking, shuffling, with hesitation. | Frontal lobe disorders (e.g., normal pressure hydrocephalus). |
| Sensory Ataxia | High-stepping gait with foot slapping due to lack of proprioception; worse in the dark. | Peripheral neuropathy, posterior column disease. |
Diagnostic Approach
1. History
- Duration, progression, associated symptoms (e.g., pain, weakness, sensory changes).
- Prior injuries, medical history (e.g., stroke, diabetes, degenerative disease).
2. Neurological Exam
- Strength, reflexes, sensation, and coordination.
- Assess for upper or lower motor neuron signs.
3. Imaging and Labs (if indicated)
- X-rays: Assess joint or bone abnormalities.
- MRI: Rule out central nervous system lesions.
- EMG/NCS: Evaluate peripheral neuropathy or radiculopathy.
Key Learning Points
- A detailed gait evaluation can localize the underlying pathology to musculoskeletal, neurological, or systemic conditions.
- Use a stepwise approach, starting with observation and specific maneuvers.
- Integrate findings with the patient’s history and physical examination for a comprehensive diagnosis.